Sunlight doesn’t just “age” skin.
It alters the systems that maintain it.
Collagen doesn’t disappear randomly, it’s broken down, mis-signalled, and rebuilt under stress. And much of that process begins with something as routine as unprotected daily light exposure.
To understand photoaging properly, you have to look beneath the surface at oxidative stress, cellular signalling, and the enzymes that quietly reshape your skin’s architecture over time.

What is Photoaging? Understanding Sun Damage Beyond the Surface
The term “photoaging” simply describes the changes in your skin caused by prolonged exposure to the sun’s radiation; primarily its ultraviolet (UV) rays, but also other forms of light [Scharffetter-Kochanek K, et al., 2000]. Think of it as skin aging accelerated by light. It’s distinct from chronological aging (the natural inevitable process of skin deterioration due to age and genetics) and accounts for a surprisingly large part of what we typically see as “signs of aging.”
Curious how enzymes like MMPs contribute to collagen breakdown and photoaging? Jump to that section.
Defining Photoaging: More Than Just a Tan
While a suntan or sunburn are immediate, visible reactions to sun exposure, photoaging is the result of long-term, cumulative damage that happens deep within your skin’s layers. The outer layer of the skin, known as the stratum corneum, acts as a protective barrier that shields the underlying tissues from the cumulative effects of sun exposure. It’s the sum of all those moments in the sun incidental exposure while driving, sitting near a window, or enjoying a cloudy day outdoors that contribute to lasting changes [Scharffetter-Kochanek K, et al., 2000].
A tan might fade, but the underlying changes to your skin’s structure and cellular DNA from repeated sun exposure can lead to more permanent concerns. Indeed, scientific reviews consistently show that up to 80-90% of visible facial aging signs can be attributed to this kind of UV exposure [Flament F, et al., 2013], highlighting just how impactful our relationship with the sun truly is.
The Culprits: UVA (the “Aging Rays”) vs. UVB (the “Burning Rays”) – Their Year-Round Impact
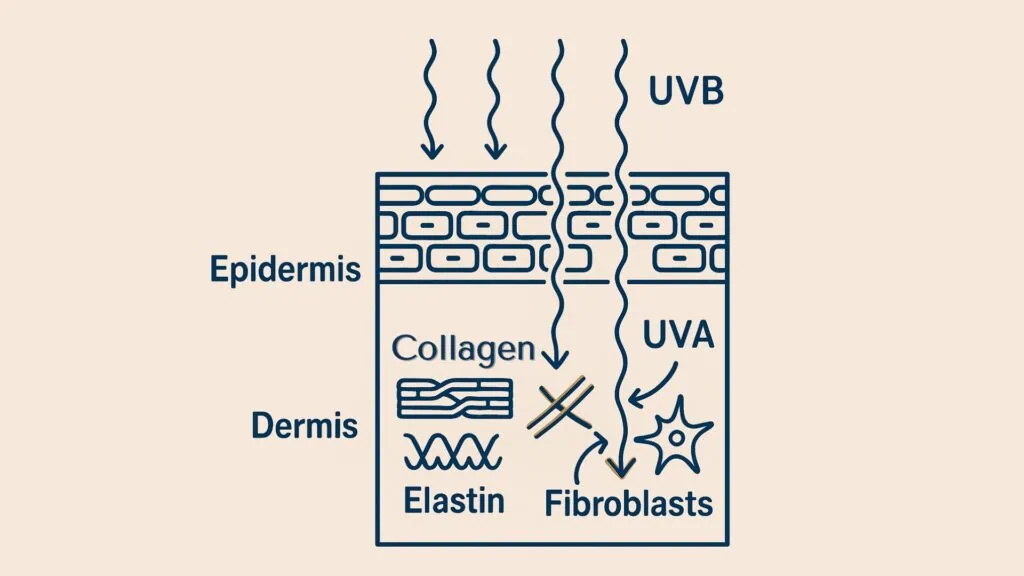
The sun’s UV radiation that reaches us is made up of two main types: UVA and UVB. They affect your skin in distinct ways:
UVB Rays (Burning Rays): These have a shorter wavelength and are mostly absorbed by the skin’s outermost layer, the epidermis. They are the primary cause of sunburn and contribute significantly to the risk of skin cancers by directly damaging DNA in skin cells [Kim T-H, et al., 2019]. UVB intensity is highest in summer and during peak sun hours, making exposure to UV from the summer sun especially risky.
UVA Rays (Aging Rays): These rays have a longer wavelength and make up about 95% of the UV radiation that gets through the atmosphere. Crucially, UVA rays penetrate much deeper into your skin, reaching down into the dermis where your skin’s vital support network, including collagen and elastin fibers [Kim T-H, et al., 2019].
Imagine UVA rays as silent saboteurs; they don’t always cause an immediate burn like UVB, but they are constantly, stealthily working beneath the surface. What makes UVA particularly insidious is its consistent presence. It’s there year-round, at the same intensity during daylight hours, regardless of whether it’s sunny or cloudy, and can even penetrate glass [Chen H, et al., 2014].
Over time, this structural disruption becomes visible, as changes in texture, elasticity, and pigmentation.
Beyond UV: Are Visible Light and Infrared Playing a Role?
While UV is the primary driver, other wavelengths such as visible light and infrared may also contribute to oxidative stress and collagen degradation, though their role is less dominants [Duteil L, et al., 2022] [Cho S, et al., 2009].
How UV Attacks Collagen from Multiple Angles and Impact Skin Barrier
UV exposure doesn’t only affect collagen, it also alters the structure of the skin barrier.
Lipid layers become depleted, and keratinocyte organisation is disrupted.
This weakens the barrier’s ability to retain moisture and regulate external stressors, increasing overall vulnerability of the skin system.
Collagen’s Crucial Role & How the Sun Wages War On It
Collagen is your skin’s primary structural protein, providing firmness and support – think of it as the skin’s supportive framework. While natural collagen production declines with age (accelerating during perimenopause and menopause [Jenkins G, et al., 2014; Zhang S & Duan E, 2018], sun exposure dramatically speeds up its loss and damage.
Collagen provides structural support, maintaining firmness, and skin elasticity. It also supports the regeneration of dead skin cells, which is vital for maintaining healthy skin. But when MMP enzymes become overactive (often due to UV stress) they accelerate collagen breakdown, undermining skin strength and resilience.
Direct Hits on Collagen Fibres: UV rays act like molecular “scissors,” directly breaking the chemical bonds within collagen and elastin fibres. This weakens your skin’s supportive “ropes,” leading to loss of strength, decreased skin elasticity, and the appearance of aged skin, including wrinkles.

Is Sun Exposure Quietly Undermining Your Repair Capacity?
Take the Nurture Assessment to see how oxidative stress and collagen renewal may be interacting in your biology.
UV radiation employs a multi-pronged attack:
Sabotaging the builders (Fibroblast Dysfunction): UV radiation damages fibroblasts, your skin’s “collagen factories.” This impairs their ability to produce new collagen and can even cause them to produce substances that further degrade existing collagen [Liu W, et al., 2024].
The Oxidative Stress Bomb
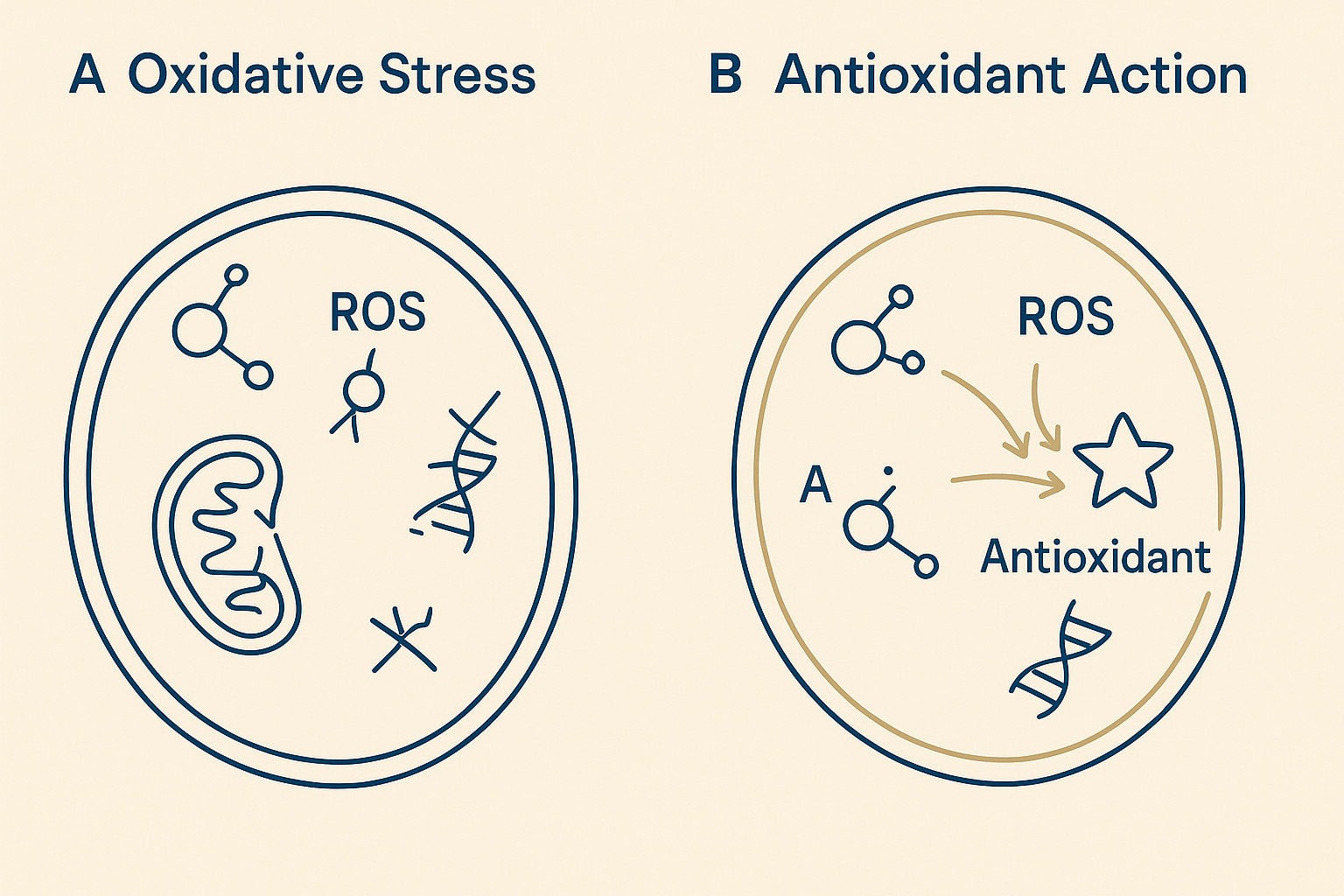
Reactive Oxygen Species (ROS): UV exposure creates a surge of unstable molecules called ROS (e.g., superoxide anions, hydroxyl radicals). Think of ROS as tiny, damaging “sparks” inside your skin.
ROS = Reactive Oxygen Species — unstable molecules that damage DNA, proteins, and lipids
Oxidative Stress: This is the harmful imbalance when there are too many ROS “sparks” for your skin’s natural antioxidant defenses to handle. This state of oxidative stress results in widespread damage that attacks collagen, cell structures, and DNA, accelerating photoaging [Puizina-Ivić N, 2013; Scharffetter-Kochanek K, et al., 2000].
Unmasking the “Hidden Accelerators”: Understanding MMPs in Skin Aging
UV exposure doesn’t just damage collagen directly, it changes the signalling environment around it.
One of the key pathways involves reactive oxygen species (ROS). These unstable molecules act as cellular stress signals, activating transcription pathways that upregulate matrix metalloproteinases (MMPs).
MMPs are not inherently harmful. They are part of normal tissue remodelling, a controlled system that clears damaged proteins. [Knox T, et al., 2024].
The problem is scale.
Under sustained UV exposure, ROS levels rise beyond what antioxidant systems can buffer. The signal becomes amplified act as internal distress signals within skin cells, initiating a chain reaction of cellular alarm bells. MMP production increases disproportionately; particularly enzymes like MMP-1 that target collagen [Scharffetter-Kochanek K, et al., 2000.; Kammeyer A & Luiten R, 2015].
What should be maintenance becomes degradation.
Collagen is broken down faster than it can be rebuilt, and the structural integrity of the dermis begins to shift.
MMPs are zinc-dependent enzymes activated through a process known as the cysteine switch. They’re kept in balance by Tissue Inhibitors of Metalloproteinases (TIMPs). It’s not the presence of MMPs that’s harmful—it’s their dysregulation under oxidative stress that disrupts skin architecture.
To support balance, antioxidants act like emergency technicians, neutralizing ROS before they can trigger excessive MMP activation.
Collagen loss in this context isn’t passive.
It reflects a shift in balance, where breakdown begins to outpace the skin’s ability to repair and maintain its structure.
That balance is regulated by signalling, enzyme activity, and the surrounding biological environment.
When this environment is disrupted, through sustained oxidative stress or dysregulated MMP activity, structural stability begins to decline over time. Explore how this system is supported in the Collagen Cofactor Complex
Addressing Sun Damage: Prevention and Repair
The first layer of intervention is behavioural: limiting excessive UV exposure and reducing cumulative oxidative stress.
But protection alone doesn’t resolve the underlying biology.
The more important question is whether the internal environment, antioxidant capacity, signalling balance, and matrix support is sufficient to maintain repair alongside exposure.
To explore how oral antioxidants provide vital internal defence, see our guide: Radiance From Within: The Science of Oral Antioxidants for Healthy, Sun-Protected Skin.
Understanding Your Skin’s Overall Defence: The Role of Antioxidant Capacity
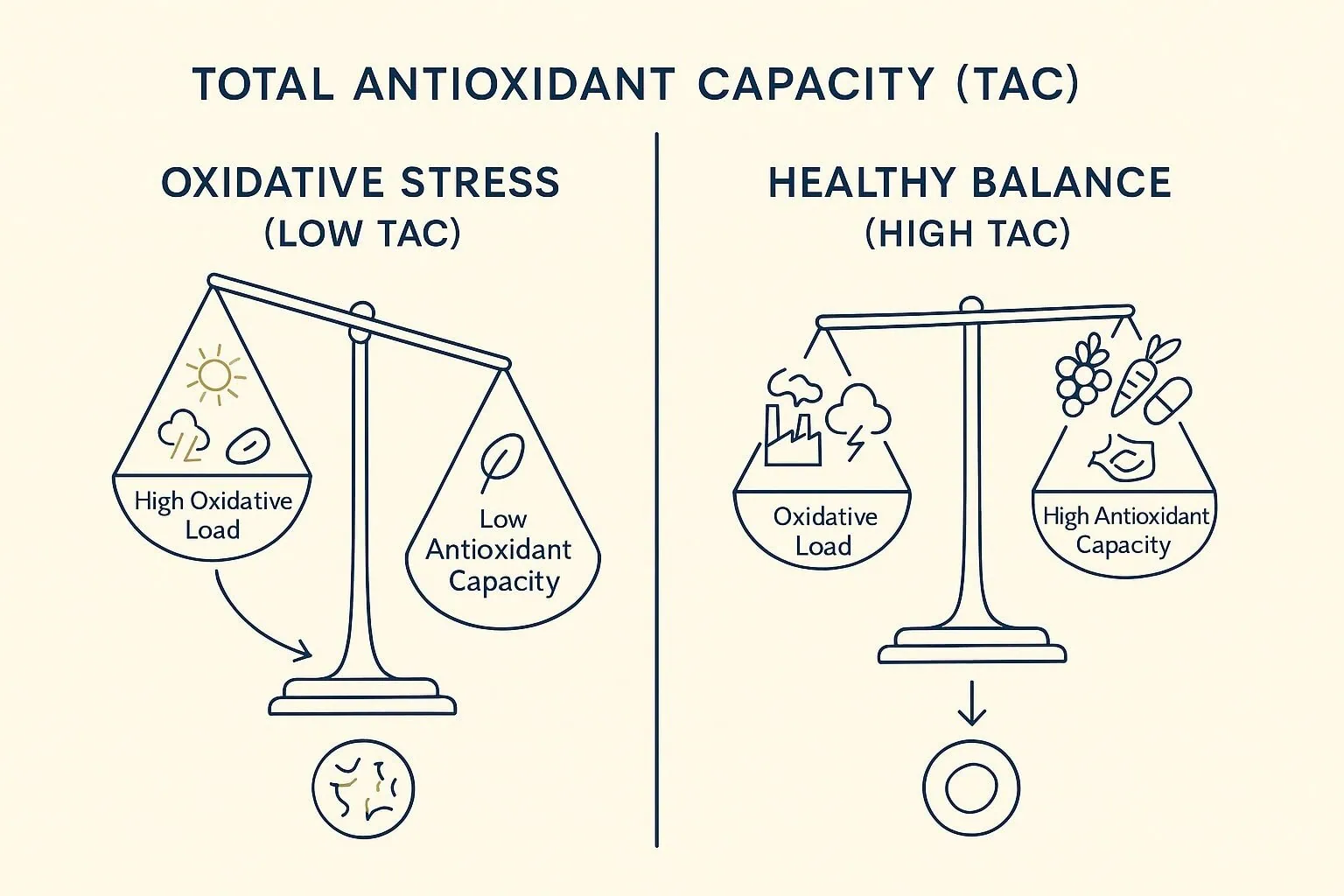
You might hear about Total Antioxidant Capacity (TAC). “What is TAC in health?” It’s the overall ability of your body and skin to neutralize harmful free radicals and combat oxidative stress. “How does TAC relate to skin health?” A robust TAC means your skin is better equipped to defend itself and repair damage.
“Can diet influence TAC and skin aging?” Yes, profoundly. What you consume significantly bolsters your systemic antioxidant defences, highlighting how an “inside-out” approach is a powerful strategy.
What Can Be Done About Sun Damage to Skin?
The sun’s impact on our skin is profound and scientifically well-documented. While natural aging is an unavoidable, genetically driven process, the accelerated effects of prolonged sun exposure and chronic sun exposure, such as photoaging, damage to elastin and collagen, and the appearance of pigmented spots can significantly worsen skin aging. From the silent work of UVA rays to the aggressive action of MMP enzymes, daily sun exposure relentlessly challenges our skin’s integrity.
Understanding these mechanisms enables you to adopt protective habits and make informed choices to nurture your skin’s health and resilience at every age.
The first line of defence is always diligent sun protection. But to truly support your skin from all angles, consider how you can bolster its internal resilience.
Ready to learn how powerful oral antioxidants can support your skin from within? Read our comprehensive guide: Radiance From Within: The Science of Oral Antioxidants for Healthy, Sun-Protected Skin.
Understand how collagen is actually rebuilt, not just supplemented.
Explore the architecture of the Collagen Cofactor Complex: a systems-level formulation designed to restore matrix integrity, support fibroblast signalling, and stabilise the biological environment collagen depends on.
Frequently Asked Questions (FAQs)
Matrix metalloproteinases (MMPs) are enzymes that naturally help remodel skin tissue, but when overactivated—often by UV exposure and oxidative stress—they break down collagen and elastin, leading to wrinkles, thinning skin, and accelerated aging.
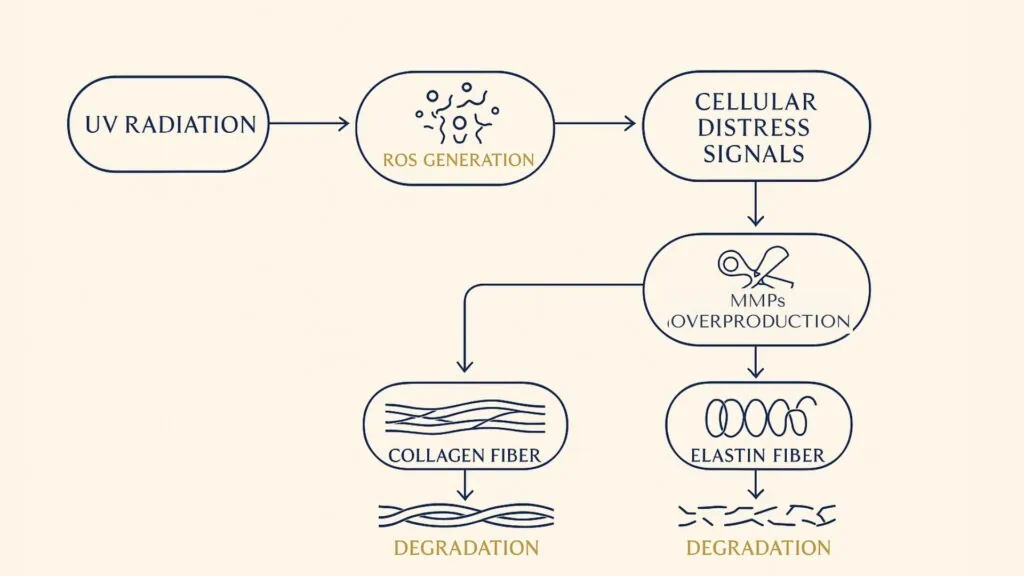
UV rays generate reactive oxygen species (ROS), which signal cells to produce more MMPs. This overproduction breaks down the skin’s support structure, contributing to visible signs of photoaging such as sagging, pigmentation, and fine lines.
MMPs are essential for natural skin repair and wound healing, but when dysregulated—due to chronic UV exposure or inflammation—they cause more harm than good by degrading structural proteins too aggressively. Balancing MMP activity is key to skin resilience.
Yes. Antioxidants like glutathione, NAC, and vitamin C neutralize ROS before they trigger excessive MMP production. This helps preserve collagen and supports healthier, firmer skin over time.